13:30
|
|
Introduction |
13:33
|
|
Chronic Obstructive Pulmonary Disease: What Does MRI Offer
Compared to CT? - Permission Withheld
Yoshiharu Ohno1,2
1Division of Functional and Diagnostic
Imaging Research, Department of Radiology, Kobe
University Graduate School of Medicine, Kobe, Japan, 2Advanced
Biomedical Imaging Research Center, Kobe University
Graduate School of Medicine, Kobe, Japan
This lecture covers 1) state of the art pulmonary MR
techniques for morphological and functional assessment,
2) its clinical applications in COPD and 3) future
direction of pulmonary functional MR imaging. We
believe that the findings of further basic studies as
well as clinical applications of this new technique will
validate the real significance of pulmonary MRI for the
future of COPD assessment and its usefulness for
diagnostic radiology and pulmonary medicine.
|
13:48
 |
0979.
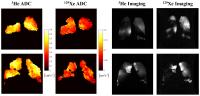 |
Comparison of 3He and 129Xe MRI for Evaluation of Lung
Microstructure and Ventilation in Healthy Volunteers and
COPD Patients at 1.5 T 
Neil James Stewart1, Ho-Fung Chan1,
Guilhem Jean Collier1, Felix Clemens Horn1,
Graham Norquay1, Juan Parra-Robles1,
Denise Yates2, Paul Collini3, Rod
Lawson4, Helen Marshall1, and Jim
Michael Wild1
1Academic Unit of Radiology, University of
Sheffield, Sheffield, United Kingdom, 2Novartis
Institutes for Biomedical Research, Cambridge, MA,
United States, 3Academic
Unit of Immunology and Infectious Diseases, University
of Sheffield, Sheffield, United Kingdom, 4Sheffield
Teaching Hospitals NHS Foundation Trust, Sheffield,
United Kingdom
3He and 129Xe
ventilation and diffusion-weighted MR images were
acquired at 1.5T in healthy volunteers and, at multiple
time-points, in COPD patients in order to compare the
functional sensitivity and assess the repeatability of
MR-derived measures of ventilated volume (VV%) and
apparent diffusion coefficient (ADC) from each of the
two gases. ADC values from both nuclei exhibited
excellent agreement and significant correlations with
pulmonary function tests (PFTs) (p<0.001), whilst VV%
values were less comparable. ADC and VV% metrics derived
from both nuclei were also shown to be repeatable, with
coefficient of variation values similar to those of
PFTs.
|
14:00
|
0980.
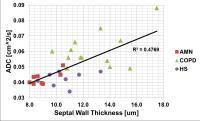 |
Discrimination of COPD Patients, Healthy Smokers and
Age-matched Normals with Hyperpolarized Xenon-129 MR
Spectroscopy 
Kai Ruppert1,2, Kun Qing2, Talissa
A. Altes2,3, and John P. Mugler III2
1Cincinnati Children's Hospital, Cincinnati,
OH, United States, 2University
of Virginia, Charlottesville, VA, United States, 3University
of Missouri, Columbia, MO, United States
Chemical Shift Saturation Recovery (CSSR) MR
Spectroscopy permits the in-vivo measurement of the
alveolar septal wall thickness (SWT) by quantifying the
uptake of hyperpolarized xenon-129 by lung parenchyma on
a millisecond timescale. In this study we correlated the
SWT with apparent diffusion coefficient (ADC)
measurements in patients with chronic-obstructive
pulmonary disease (COPD), healthy smokers and
age-matched normals. While the ADC measurements and
conventional pulmonary function tests could detect
statistically significant differences between the COPD
and non-COPD subjects, only CSSR spectroscopy could, in
addition, discriminate healthy smokers from the
age-matched normals.
|
14:12
|
|
Imaging Lung Cancer: MRI, PET or Both? 
Nina F Schwenzer1
1Dept. of Radiology, University Hospital
Tübingen
Whereas CT is mainly used for local staging, PET/CT
offers additional information about tumor metabolism and
distant metastases. Although MRI is still limited in the
detection of small lung nodules it offers additional
functional information about diffusion and perfusion of
tumor masses. In the framework of personalized medicine
imaging has evolved from localizing disease towards
prognostic and predictive biomarkers as well as
treatment response. Hybrid modalities (PET/CT and
PET/MRI) have the potential to offer a broad variety of
parameters (i.e. textural parameters and multiparametric
information) which can be used for further analyses such
as radiomics or radiogenomics.
|
14:27
|
0981.
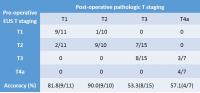 |
A comparison between free-breathing radial VIBE in 3T MR and
endoscopic ultrasound for preoperative T staging of
potentially resectable esophageal cancer with
histopathological correlation 
Jinrong Qu1,2, Hui Liu3, Zhaoqi
Wang2, Ihab R Kamel4, Kiefer
Berthold5, Robert Grimm5,6,
Jianjun Qin7, and Hailiang Li1
1Radiology, Henan Cancer Hospital, Zhengzhou,
China, People's Republic of, 2Radiology,
the affiliated Cancer Hospital of Zhengzhou University,
Zhengzhou, China, People's Republic of, 3MR
Collaboration, Siemens Healthcare, Shanghai, China,
People's Republic of, 4Radiology,
Johns Hopkins University School of Medicine, Baltimore,
MD, United States, 5MR
Pre-development, Siemens Healthcare, Erlangen, Germany, 6Erlangen,
Germany, 7Thoracic
surgery, Henan Cancer Hospital, Zhengzhou, China,
People's Republic of
Contrast-enhanced free-breathing r-VIBE is superior to
EUS in T staging of potentially resectable EC, not only
for T1 and T2, but also for T3 and T4.
|
14:39
|
0982.
|
Evaluating tumor biology of lung adenocarcinoma:
multimodality-multiparametric approach - Permission Withheld
Ho Yun Lee1, Seong-Yoon Yun Ryu1,
Ji Yun Jeong2, Kyung Soo Lee1, and
Young Mog Shim3
1Samsung Medical Center, Sungkyunkwan
University School of Medicine, Seoul, Korea, Republic
of, 2Pathology,
Kyungpook National University Medical Center, Kyungpook
National University School of Medicine, Daegu, Korea,
Republic of, 3Thoracic
Surgery, Samsung Medical Center, Sungkyunkwan University
School of Medicine, Seoul, Korea, Republic of
Our purpose is to investigate tumor biology of lung adenocarcinoma such
as tumor cellularity, characteristics of invasion,
histologic subtype, and tumor differentiation using
multimodality and multiparametric imaging approach.
SUVmax was significantly greater in the solid subtype
and poorly differentiated tumor when compared to other
subtypes or differentiations. f tended to increase as
tumor differentiation changed more poorly, whereas D and
D * showed a trend of decrease in poorly differentiated
tumors. Tumor size, the size of the solid portion within
the tumor, and ADC showed significant correlation with
extent of tumor invasion. SUVmax showed significant
correlation with tumor cellularity.
|
14:51
|
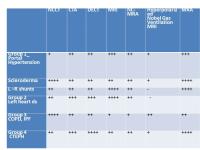 |
Imaging of Pulmonary Vascular Disease: Can MRI Replace CT? 
Mark Schiebler1
1UW=Madison
MRI methods have become increasingly relied upon by
pulmonary medicine and cardiovascular medicine to help
diagnose pulmonary hypertension and monitor the effects
of therapy on the right ventricle. Recently selected
sites have begun using MRA for the primary diagnosis of
pulmonary embolism. This symposium will discuss the
highlights and difficulties in the use of MRI for the
diagnosis and follow up of pulmonary vascular diseases.
|
15:06
 |
0983.
 |
Quantification of lung parenchyma perfusion in small animal
imaging with Flow-sensitive Alternating Inversion Recovery
(FAIR) 2D UTE 
Marta Tibiletti1, Andrea Bianchi2,
Detlef Stiller2, and Volker Rasche1,3
1Core Facility Small Animal MRI, Ulm
University, Ulm, Germany, 2Target
Discovery Research, In-vivo imaging laboratory,
Boehringer Ingelheim Pharma GmbH & Co. KG, Biberach an
der Riss, Germany, 3Department
of Internal Medicine II, Ulm University, Ulm, Germany
Functional information of the lung is of great
importance for staging and monitoring lung disease. In
this context, perfusion is conventionally addressed by
systemic injection of contrast agent (CA) with
subsequent quantitatively monitoring of the wash-in of
the CA, or more frequently qualitatively assessment of
the lung intensity pattern during the CA steady-state
phase. Especially in small animal imaging,
quantification of the respective perfusion dynamics is
difficult due to the rather coarse temporal resolution
achievable. In this work, the application of the
non-invasive FAIR technique is combined with a 2D UTE
readout thus enabling non-invasive quantification of
lung perfusion.
|
15:18
|
0984.
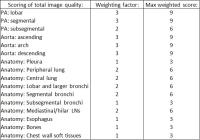 |
Comparison of Pulmonary Magnetic Resonance Angiography (MRA)
and free-breathing Ultra short time to echo (UTE) for the
comprehensive evaluation of the vascular and non-vascular
anatomy of the chest 
Julie A Bauml1, Mark L Schiebler1,
Christopher J Francois1, Kevin M Johnson2,
and Scott K Nagle1,2,3
1Radiology, University of Wisconsin Madison,
Madison, WI, United States, 2Medical
Physics, University of Wisconsin Madison, Madison, WI,
United States, 3Pediatrics,
University of Wisconsin Madison, Madison, WI, United
States
MR imaging of the chest is challenging due to the low
proton density, the short T2* of the lungs and
cardiorespiratory motion. Many patients suspected of
pulmonary embolism are short of breath, which can limit
the utility of breath-held techniques. Free-breathing
ultrashort echo time (UTE) approaches (TE < 0.10 ms)
help to overcome some of these difficulties. In this
prospective pilot clinical study, we demonstrate that
UTE provides better overall depiction of chest
structures when compared to MRA. We conclude that UTE is
complementary to MRA of the chest in the analysis of
both vascular and non-vascular thoracic structures.
|
15:30
|
|
Adjournment & Meet the
Teachers |
|








