10:00
|
|
Introduction by Moderator |
10:03
|
|
Fat Quantification & Composition 
Mustafa Bashir1
1Duke University Medical Center
The use of MRI measures of fatty liver as well as
intraabdominal fat will be discussed, particularly as
pertain to Nonalcoholic Steatohepatitis and the
metabolic syndrome.
|
10:18
|
0357.
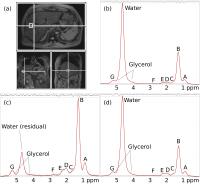 |
Non-invasive quantification and characterisation of liver
fat in non-alcoholic fatty liver disease (NAFLD) using
automated analysis of MRS correlated with histology 
Robert Flintham1, Peter Eddowes2,
Scott Semple3, Natasha McDonald4,
Jonathan Fallowfield4, Tim Kendall5,
Stefan Hübscher6, Philip Newsome2,
Gideon Hirschfield2, and Nigel Paul Davies1,7
1Medical Physics, University Hospitals
Birmingham NHS Foundation Trust, Birmingham, United
Kingdom, 2Centre
for Liver Research, NIHR Biomedical Research Unit,
University of Birmingham, Birmingham, United Kingdom, 3Clinical
Research Imaging Centre, University of Edinburgh,
Edinburgh, United Kingdom, 4MRC
Centre for Inflammation Research, University of
Edinburgh, Edinburgh, United Kingdom, 5MRC
Human Genetics Unit, University of Edinburgh, Edinburgh,
United Kingdom, 6Pathology,
University Hospitals Birmingham NHS Foundation Trust,
Birmingham, United Kingdom, 7Institute
of Cancer and Genomics, University of Birmingham,
Birmingham, United Kingdom
MRS is proven to accurately measure liver fat fraction
(FF), but its potential to differentiate steatohepatitis
from simple steatosis in non-alcohol related fatty liver
disease (NAFLD) is unexplored. MRS was acquired in 60
patients with suspected NAFLD across two centres prior
to biopsy. Automated analysis was developed using
TARQUIN to estimate FF, lipid chain length (CL) and
number of double-bonds per chain (nDB) revealing strong
correlations between FF, nDB, CL and steatosis grade.
nDB also negatively correlated with hepatocyte
ballooning assessed by histopathology. Further
investigation of the relationship between MRS-derived
lipid composition measurements and disease severity in
NAFLD is warranted.
|
10:30
|
0358.
 |
Accuracy and optimal proton density fat fraction threshold
of magnitude- and complex-based magnetic resonance imaging
for diagnosis of hepatic steatosis in obese patients using
histology as reference 
Tydus Thai1, William Haufe1,
Yesenia Covarrubias1, Alexandria Schlein1,
Curtis N. Wiens2, Alan McMillan2,
Nathan S. Artz2,3, Rashmi Agni4,
Michael Peterson5, Luke Funk6,
Guilherme M. Campos7, Jacob Greenberg6,
Santiago Horgan8, Garth Jacobson8,
Tanya Wolfson1, Jeffrey Schwimmer9,
Scott Reeder2,10,11,12,13, and Claude Sirlin1
1Liver Imaging Group, Radiology, University
of California-San Diego, San Diego, CA, United States, 2Radiology,
University of Wisconsin-Madison, Madison, WI, United
States, 3Radiological
Sciences, St. Jude Children's Research Hospital,
Memphis, TN, United States, 4Pathology,
University of Wisconsin-Madison, Madison, WI, United
States, 5Western
Washington Pathology and Multicare Health System,
Tacoma, WA, United States,6Surgery,
University of Wisconsin-Madison, Madison, WI, United
States, 7Surgery,
Virginia Commonwealth University, Richmond, VA, United
States, 8Surgery,
University of California-San Diego, San Diego, CA,
United States, 9Pediatrics,
University of California-San Diego, San Diego, CA,
United States, 10Medical
Physics, University of Wisconsin-Madison, Madison, WI,
United States, 11Biomedical
Engineering, Madison, WI, United States, 12Medicine,
Madison, WI, United States, 13Emergency
Medicine, Madison, WI, United States
The purpose of this prospective cross-sectional study
was to determine the accuracy of optimal MRI-M- and
MRI-C-determined PDFF thresholds for diagnosis of
hepatic steatosis using contemporaneous histology as
reference in obese adults without previously known
NAFLD. The excellent performance parameters of the
Youden-index PDFF thresholds for MRI-M and MRI-C (5.3%
and 7.7%, respectively) further support the use of these
techniques for the quantitative and non-invasive
diagnosis of HS. If validated by additional prospective
studies, these PDFF thresholds could be used for
diagnosing HS in obese adults non-invasively.
|
10:42
|
|
Confounders to Iron Quantification in the Liver 
Diego Hernando1
1University of Wisconsin-Madison, WI, United
States
This presentation will provide an overview of current
techniques for liver iron quantification, with a focus
on relevant confounding factors which may decrease the
accuracy and reproducibility of LIC estimates. The
effect of these confounders, as well as recent efforts
to address them, will be presented.
|
10:57
 |
0359.
 |
Iron overload quantification using UTE Imaging at 3T 
Eamon K Doyle, MS1,2, Jonathan M Chia, MS3,
and John C Wood, MD, PhD1,2
1Biomedical Engineering, University of
Southern California, Los Angeles, CA, United States, 2Cardiology,
Children's Hospital of Los Angeles, Los Angeles, CA,
United States, 3Philips
Healthcare, Cleveland, OH, United States
Estimate of R2* in high-iron patients has many
challenges at 3T and above. UTE imaging shows promise
as method to perform iron quantitation in heavily
iron-loaded tissues. We demonstrate feasibility of
using a 3D radial UTE sequence at 3T to estimate R2*
relaxation rates in iron-loaded human subjects and
fast-decay phantoms.
|
11:09
|
0360.
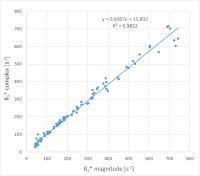 |
Comparing Magnitude versus Complex Data Fitting in Liver R2*
Relaxometry 
Arthur Peter Wunderlich1,2, Stefan Andreas
Schmidt1, Meinrad Beer1, Armin
Michael Nagel1,2, and Holger Cario3
1Clinic for Diagnsotic and Interventional
Radiology, Ulm University, Medical Center, Ulm, Germany, 2Section
for Experimental Radiology, Ulm University, Medical
Center, Ulm, Germany, 3Department
of Pediatrics and Adolescent Medicine, Ulm University,
Medical Center, Ulm, Germany
Relaxometry of patient data was performed comparing the
use of magnitude versus complex data. 94 patients
suspected for liver iron overload were scanned with
mulit-contrast GRE-MRI at 1.5 T, involving multiple TE,
TR and
FA. Analysis was performed as conjoined fit
incorporating effects of fat/water dephasing. One fit
was based on magnitude images modeling noise as free fit
parameter, the other on complex data. Magnitude fit
yielded similar results, but showed superior convergence
and lower result uncertainty compared to the approach
involving complex data.
|
11:21
|
|
Fibrosis: MRI vs US Elastography 
Meng Yin
Liver stiffness now a well-established biomarker for
assessing fibrosis in chronic liver disease, as an
alternative to biopsy. MRI-based and ultrasound-based
dynamic elastography methods have been introduced for
clinical staging of fibrosis. Some of the methods are
commercially available. However, each have their
inherent strengths and weaknesses. The published
literature generally indicates that MR elastography has
higher diagnostic performance and fewer technical
failures than ultrasound-based elastography in assessing
hepatic fibrosis. There is significant potential to
further develop elastography techniques to implement
multiparametric methods that have promise for
distinguishing between process such as inflammation,
fibrosis, venous congestion, etc.
|
11:36
|
0361.
 |
Discrimination of Hepatic Inflammation and Fibrosis with
Magnetic Resonance Elastography 
Meng Yin1, Kevin J. Glaser1,
Harmeet Malhi2, Amy Mauer2,
Anuradha Krishnan2, Taofic Mounajjed3,
Jason Bakeberg4, Christopher Ward4,
Ruisi Wang2, Douglas Simonnetto2,
Shennen Mao5, Jaime Glorioso5,
Faysal Elgilani6, Vijay Shah2,
Scott Nyberg6, Armando Manduca1,
and Richard L. Ehman1
1Radiology, Mayo Clinic, Rochester, MN,
United States, 2Gastroenterology
and Hepatology, Mayo Clinic, Rochester, MN, United
States, 3Pathology,
Mayo Clinic, Rochester, MN, United States, 4Nephrology
and Hypertension Research, Mayo Clinic, Rochester, MN,
United States, 5Surgery,
Mayo Clinic, Rochester, MN, United States, 6Transplant
Center, Mayo Clinic, Rochester, MN, United States
To investigate the utility of MRE-derived mechanical
properties in discriminating hepatic inflammation and
fibrosis in early-stage of chronic liver diseases, we
performed multifrequency 3D MRE on five different in
vivo animal
models with chronic liver diseases. Liver stiffness and
phase angle derived from complex shear modulus were
selected for evaluation. Results demonstrated distinct
and potentially characteristic changes in these
mechanical properties with hepatic inflammation,
fibrosis and increased portal pressure. The findings
offer preliminary evidence of the potential to extend
MRE to distinguish and independently assess
necroinflammatory and fibrotic processes in the early
phase of chronic liver diseases.
|
11:48
|
0362.
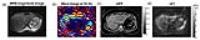 |
Multifrequency MR elastography for assessing hepatic
fibrosis in pediatric non-alcoholic fatty liver disease 
Jing Guo1, Christian Hudert2,
Heiko Tzschätzsch1, Andreas Fehlner1,
Florian Dittmann1, Jürgen Braun3,
and Ingolf Sack1
1Radiology, Charité - Universitätsmedizin
Berlin, Berlin, Germany, 2Charité
- Universitätsmedizin Berlin, Berlin, Germany, 3Department
of Medical Informatics, Charité - Universitätsmedizin
Berlin, Berlin, Germany
Multifrequency MR elastography (MMRE) was applied to 32
obese pediatric patients with non-alcoholic fatty liver
disease (NAFLD). Magnitude shear modulus |G*|
which relates to liver stiffness is sensitive to
differentiate mild fibrosis (F0-2) from severe fibrosis
(F3) with an AUROC of 0.93. The liver stiffness was
positively correlated with serum alanine
aminotransferase (ALT) and can potentially serve as a
quantitative imaging marker for the noninvasive
assessment of liver fibrosis in patients with NAFLD.
|
12:00
|
|
Adjournment & Meet the
Teachers |
|






