Oral
Body: Breast, Chest, Abdomen, Pelvis
Thursday, 27 April 2017
| Room 320 |
13:00 - 15:00 |
Moderators: Scott Nagle, Edwin VanBeek |
Slack Channel: #s_body
Session Number: O33
13:00
|
1182.
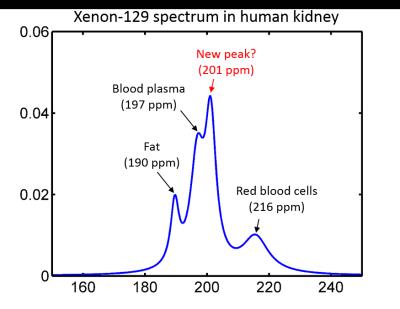 |
Dynamic Spectroscopy of Dissolved-Phase Xenon-129 in the Human Kidney - permission withheld
G. Miller, Gordon Cates Jr., David Keder, Talissa Altes, Jaime Mata, Kun Qing, Iulian Ruset, F. Hersman, John Mugler III
The increase in available dissolved-phase signal made possible by high-performing Xe-129 polarizers has led to renewed interest in dissolved-phase imaging of Xe-129 outside the lung. Here we examine the time course of the dissolved phase Xe-129 signal in the human kidney following gas inhalation, in order to optimize kidney image acquisition and explore the potential for studying kidney function using hyperpolarized Xe-129. In addition to spectral peaks commonly associated with Xe-129 dissolved in tissue/plasma, red blood cells, and fat, we have identified an additional peak at 201 ppm that lags the blood peaks by a few seconds.
|
13:12
 |
1183.
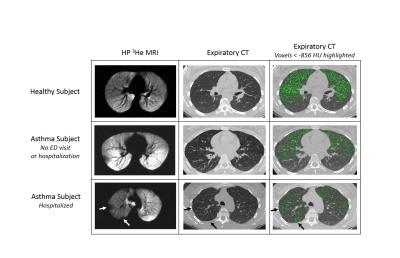 |
Ventilation Defect Percent in Helium-3 MRI is Associated with Severe Outcomes in Asthma 
David Mummy, Stanley Kruger, Michael Evans, Wei Zha, Ronald Sorkness, Nizar Jarjour, Mark Schiebler, Loren Denlinger, Sean Fain
We assessed the ventilation defect percent (VDP) on hyperpolarized helium-3 MRI as an indicator of severe clinical outcomes (emergency department [ED] visits and hospitalizations as surrogates for significant asthma exacerbations). We compared VDP with conventional biomarkers of lung function and inflammation and found VDP was more strongly associated with both ED and hospitalizations as outcomes. VDP was correlated with spirometry, air trapping measured on CT, and eosinophil levels in sputum and peripheral blood. These findings suggest that VDP is a candidate biomarker associated with clinical outcomes of asthma exacerbation and stability.
|
13:24
 |
1184.
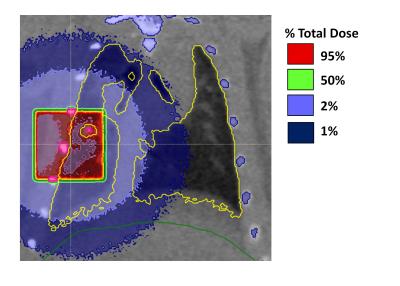 |
Regional Detection of Lung Injury using Hyperpolarized Xenon-129 Mapping of Blood Hematocrit in a Rat Model Involving Partial-Lung Irradiation 
Brandon Zanette, Elaine Stirrat, Salomeh Jelveh, Andrew Hope, Giles Santyr
Dissolved 129Xe imaging holds promise for the detection of early functional decline due to radiation-induced lung injury through the extraction of regional quantitative parameters relating to lung physiology and gas exchange. In this work a spiral-IDEAL imaging technique was used with a partial-lung irradiation rat model to investigate regional changes lung function associated with injury and compare to histology. A significant reduction in capillary hematocrit (HCT) was observed in the vicinity of irradiation. These results were in agreement with quantitative histology of red blood cells. Imaging results were more sensitive than whole-lung spectroscopy, which was performed simultaneously.
|
13:36
|
1185.
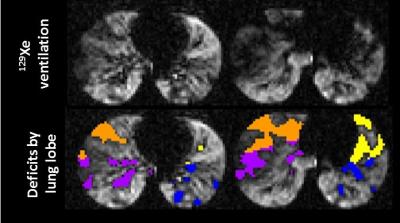 |
Ventilation heterogeneity of pediatric cystic fibrosis accessed via lung clearance index and hyperpolarized 129Xe MRI 
Laura Walkup, Robert Thomen, Emily Bell, Beth Decker, Zackary Cleveland, John Clancy, Jason Woods
Quantitative hyperpolarized 129Xe ventilation MRI was compared to FEV1, the spriometric gold standard for assessing lung function, and lung clearance index (LCI), an emerging pulmonary function test to assess global ventilation heterogeneity, in 12 pediatric cystic fibrosis subjects. A range of severity and spatial distributions of 129Xe ventilation deficits were observed, with a 129Xe ventilation defect percentage (VDP) of 18.0% ± 8.1%. VDP did not correlate with FEV1 (p=0.45) but correlated very strongly with LCI (p=0.0001), suggesting that the spatial distribution of defects in the 129Xe images represents obstructed areas of the lung that give rise to elevated LCI.
|
13:48
 |
1186.
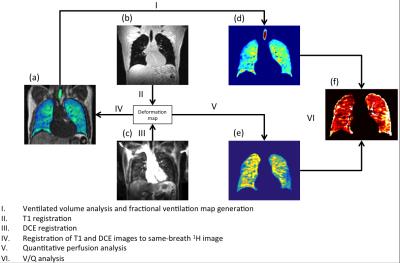 |
Quantitative ventilation-perfusion imaging using co-registered hyperpolarized gas and contrast enhanced 1H perfusion MRI 
Paul Hughes, Bilal Tahir, Felix Horn, Alberto Biancardi, Rob Ireland, Helen Marshall, Jim Wild
Analysis of the matching of ventilation and perfusion using MRI is an important area of research in the pulmonary MRI community. This work presents a quantitative method of voxelwise analysis of ventilation from hyperpolarized gas MRI and perfusion from dynamic contrast enhanced 1H MRI. The method developed allows for direct comparison of ventilation and perfusion including global measurements of ventilated and perfused volume.
|
14:00
|
1187.
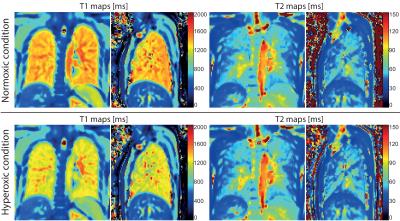 |
Oxygen-enhanced pulmonary relaxometry using ultra-fast steady-state free precession imaging 
Grzegorz Bauman, Orso Pusterla, Francesco Santini, Oliver Bieri
This study demonstrates the feasibility of fast and simultaneous T1 and T2 mapping of the lung parenchyma in oxygen-enhanced MRI. The data acquisition was performed using an adapted 2D inversion recovery ultra-fast steady-state free precession imaging in healthy human subjects. Relaxation time maps were generated for normoxic and hyperoxic acquisitions. Statistical analysis was performed to compare the relaxation times in the lung parenchyma for both gas conditions.
|
14:12
|
1188.
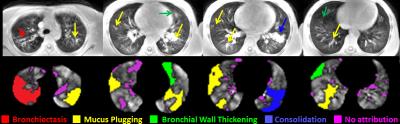 |
Investigating regional pulmonary structure-function relationships using hyperpolarized 129Xe MRI and ultra-short echo-time MRI 
Robert Thomen, Laura Walkup, David Roach, Zackary Cleveland, John Clancy, Jason Woods
We have quantified the extent of ventilation impairment in lungs due to specific pathologies associated with cystic fibrosis (CF) lung disease using ultrashort echo-time (UTE) MRI to identify structural abnormalities and hyperpolarized (HP) 129Xe MRI to identify ventilation deficits. We found that bronchiectasis demonstrates the best correlation with lung function decline, as measured by the percent predicted forced expiratory volume in 1 second (FEV1% predicted) and demonstrated the greatest deficit in HP 129Xe signal within corresponding defective regions. However, the greatest volume-percentage of defects identified were due to mucus plugging.
|
14:24
|
1189.
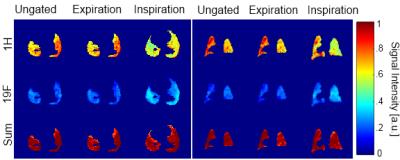 |
Respiratory self-gating and estimation of gas/proton fractions in SF6 and proton lung imaging in free-breathing mice 
Marta Tibiletti, Volker Rasche
Fluorinated gases are a promising alternative to hyperpolarized gases to study ventilation in clinical and preclinical applications. 3D Ultra Short Echo Time (UTE) acquisitions can be employed to visualize inhaled SF6 and lung parenchyma. DC self-gating was applied to discriminate between inspiration and expiration in free-breathing acquisitions. Proton and gas density were estimated in inspiration, expiration and in ungated data. The information derived from tissue-density changes matched the changes observed in the gas density, thus indicating the ventilation information can be derived from tissue density mapping.
|
14:36
 |
1190.
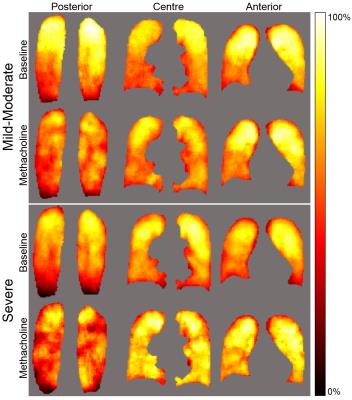 |
Pulmonary MRI Ventilation Defects in Asthma: Stochastic or Deterministic? 
Rachel Eddy, Dante Capaldi, Khadija Sheikh, Sarah Svenningsen, David McCormack, Grace Parraga
Pulmonary MRI provides strong evidence of ventilation abnormalities that are temporally and spatially persistent; this has generated a paradigm shift in our understanding of asthma as a spatially and temporally heterogeneous, non-stochastic disease. Based on these findings, here our objective was to develop image-processing methods to estimate and mathematically describe the spatial probability distribution of MRI-derived ventilation defects. To accomplish this, we generated functional lung MRI atlases based on asthmatics who were evaluated before and post-methacholine using hyperpolarized 3He static-ventilation MRI. This proof-of-concept evaluation showed that in asthmatics, ventilation abnormalities are not diffuse nor stochastic, but heterogeneous and deterministic.
|
14:48
|
1191.
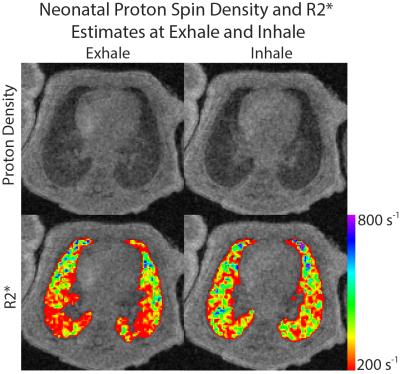 |
Proton Density and R2* Estimation of Neonatal Lung Parenchyma During Free Breathing with UTE MRI 
Andrew Hahn, Nara Higano, Jean Tkach, Laura Walkup, Robert Thomen, Xuefeng Cao, Stephanie Merhar, Jason Woods, Sean Fain
The majority of patients in the neonatal intensive care unit (NICU) have pulmonary morbidities, yet little is known about the underlying parenchymal structure. We quantify parenchymal proton density and R2* in the lungs of quiet breathing, non-sedated neonates in the NICU using a multi-echo 3D radial UTE MRI. Results indicate that lung proton density decreases as expected with lung inflation, while R2* increases. A positive relationship between gravitational dependence and tissue density is also apparent, while R2* decreases in more gravitationally dependent regions. Overall, our findings support a negative relationship between tissue density and R2* in the neonatal lung.
|
|












