Oral
Neurofluids & Brain Waste Clearance Imaging
ISMRM & SMRT Annual Meeting • 15-20 May 2021

| Concurrent 6 | 16:00 - 18:00 | Moderators: Petrice Cogswell & Kristina Sonnabend |
 |
0377.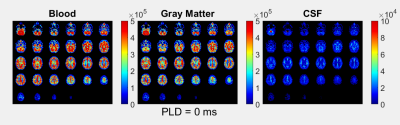 |
Blood-CSF Barrier Imaging in the Human Brain with Arterial Spin Labeling
Leonie Petitclerc1,2, Lydiane Hirschler1, Jack A. Wells3, David L. Thomas4,5,6, and Matthias J.P. van Osch1,2
1C.J. Gorter Center for High Field MRI, Department of Radiology, Leiden University Medical Center, Leiden, Netherlands, 2Leiden Institute for Brain and Cognition (LIBC), Leiden, Netherlands, 3UCL Centre for Advanced Biomedical Imaging, Division of Medicine, University College London, London, United Kingdom, 4Neuroradiological Academic Unit, Department of Brain Repair and Rehabilitation, UCL Queen Square Institute of Neurology, University College London, London, United Kingdom, 5Dementia Research Centre, UCL Queen Square Institute of Neurology, University College London, London, United Kingdom, 6Wellcome Centre for Human Neuroimaging, UCL Queen Square Institute of Neurology, University College London, London, United Kingdom
In order to measure the function of the blood-CSF barrier (BCSFB), a modified ASL experiment is introduced. This is accomplished with multiple time-points, including long labeling duration and post-labeling delay, and an echo train of 8 TEs from 10-1837ms. Long-T2 ASL signal, attributable to the CSF, was found both in the choroid plexus and around the cortex. Fitting of this signal to two models (a simple triexponential and a dynamic compartmental model) reveals an amount of CSF signal about 5 times lower than the perfusion. The transfer time of water across the BCSFB is estimated at around 100s.
|
|
0378.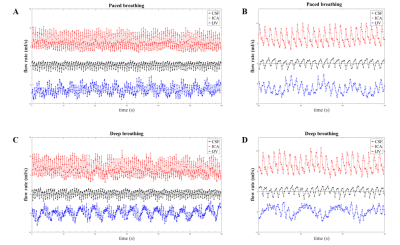 |
Arterial, venous and cerebrospinal fluid flow oscillations in real-time phase contrast MRI: type of breathing matters
Maria Marcella Lagana1, Noam Alperin2, Laura Pelizzari1, Ning Jin3, Domenico Zaca4, Marta Cazzoli1, Giuseppe Baselli5, and Francesca Baglio1
1CADiTeR, IRCCS Fondazione Don Carlo Gnocchi ONLUS, Milan, Italy, 2University of Miami, Miami, FL, United States, 3MR R&D Collaborations, Siemens Medical Solutions USA, Inc., Cleveland, OH, United States, 4Siemens Healthcare, Milan, Italy, 5Department of Electronics, Information, and Bioengineering, Politecnico di Milano, Milan, Italy
We used real-time phase contrast MRI for assessing the cardiac and respiratory influence on the neck arterial and venous flows, and on the cervical cerebrospinal fluid (CSF) flow. Changes due to the type of breathing were investigated acquiring six healthy volunteers for 60s during normal and deep breathing. The power spectra were computed from the flow rates. Two main peaks, corresponding to the breathing rate (BR) and the heart rate (HR), were found. Comparing deep breathing to normal breathing, we observed the following trends: decrement of average blood flow rates; reversal of average CSF flow rate; increment of BR power.
|
||
0379.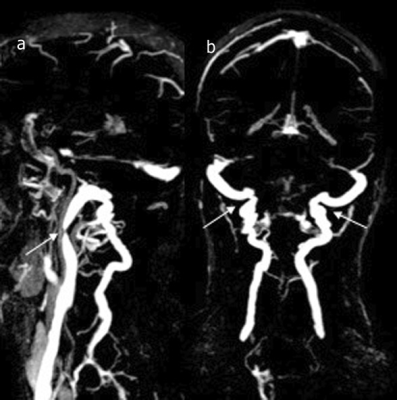 |
Phase contrast MRI analysis of neurofluids in patients with Meniere’s disease and jugular venous stenosis.
Nivedita Agarwal1, Olivier Baledent2, Giuseppe Nicolò Frau3, and Sabino Walter Della Sala1
1Radiology, APSS Ospedale Santa Maria del Carmine, Rovereto, Italy, 2University of Amiens, Amiens, France, 3Otorhinolaryngology, APSS Ospedale Santa Maria del Carmine, Rovereto, Italy
Meniere’s disease patients have a high incidence of abnormal neck venous vessels. An inefficient intracranial venous outflow would disturb global neurofluids dynamics and alter intracranial pressure. We used phase contrast MRI to correlate the dynamics of total arterial, total venous and CSF with morphological alterations in internal jugular veins (IJV). Our results show that although >80% of patients have IJV stenosis and isolated CSF and/or blood flow abnormalities, the global neurofluid dynamics remained unhampered. These results underscore the optimal compensation provided by collateral venous pathways and suggests that PC-MRI is an important adjunct clinical tool to to study neurofluids dynamics.
|
||
0380.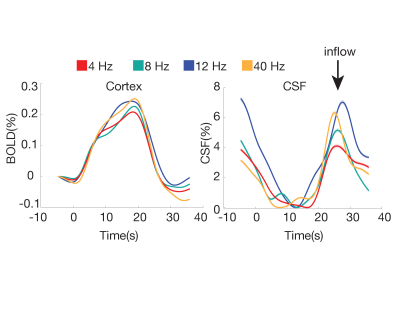 |
Visually-evoked cerebrospinal fluid flow in the human brain during wakefulness
Stephanie D Williams1, Nina E Fultz2, Nicole Tacugue3, Zenia Valdiviezo3, and Laura D Lewis2
1Psychological and Brain Sciences, Boston University, Boston, MA, United States, 2Biomedical Engineering, Boston University, Boston, MA, United States, 3Boston University, Boston, MA, United States
Cerebrospinal fluid (CSF) flow is essential for brain health, and previous studies have shown that it is driven by systemic physiological factors, such as breathing. Recent work has shown that neural activity is coupled to CSF flow during sleep, but whether this relationship reflects a causal link has not been tested. Here we investigated whether driving neural activity can induce changes in CSF flow. We found that we could induce CSF flow in the human brain during the awake state by manipulating hemodynamics with stimulus-evoked neural activity.
|
||
0381.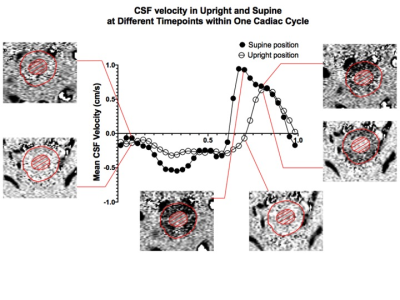 |
Upright vs. Supine MRI: Effects of body position on craniocervical CSF flow
Marco Muccio1, David Chu2, Lawrence Minkoff2, Neeraj Kukarni2, Brianna Damadian2, Raymond Damadian2, and Yulin Ge1
1Department of Radiology, New York University Grossman School of Medicine, New York City, NY, United States, 2FONAR Corporation, Melville, NY, United States
CSF exchange between the spinal cord and the cranium increases in asymptomatic human subjects when body position is shifted from upright to supine. This appears to be caused by an increase in CSF flow during diastole, in the caudo-cranial direction, and systole, in cranio-caudal direction. Extrapolation of the results showed that within a 24 hour timescale, the more time spent in the supine position (asleep) correlated with more CSF exchanged between the spinal cord and the intracranial space. These alterations can therefore play a major role in brain waste clearance, and possibly many neurodegenerative diseases as well as age-related ailments.
|
||
 |
0382.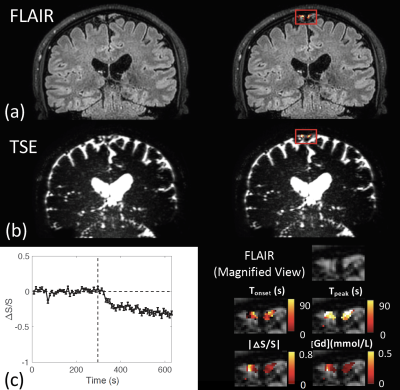 |
Fast whole brain MR imaging of dynamic susceptibility contrast changes in the CSF (cDSC MRI)
Di Cao1,2, Ningdong Kang1, Jay J. Pillai1, Xinyuan Miao1,2, Adrian Paez2, Xiang Xu1,2, Jiadi Xu1,2, Xu Li1,2, Qin Qin1,2, Peter C.M. Van Zijl1,2, Peter Barker1, and Jun Hua1,2
1Johns Hopkins University, Baltimore, MD, United States, 2Kennedy Krieger Institute, Baltimore, MD, United States
The circulation of cerebrospinal fluid (CSF) influences various aspects of brain physiology. This study aims to develop and optimize MRI sequences that can detect dynamic signal changes in the CSF after Gd administration with a sub-millimeter spatial resolution, temporal resolution of <10s, and whole brain coverage. Bloch simulations were performed to determine optimal imaging parameters. Simulations were validated with phantom scans. An optimized turbo-spin-echo (TSE) sequence was performed on healthy volunteers on 3T and 7T. In human scans, dynamic signal changes after Gd injection in the CSF were detected at location where cerebral lymphatic vessels were identified in previous studies.
|
|
0383.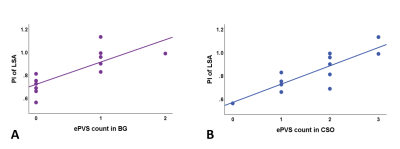 |
The association of intracranial arterial pulsatility with enlarged perivascular spaces
M. van den Kerkhof1,2, M.M. van der Thiel1,2, I.H.G.B. Ramakers2,3, R.J. van Oostenbrugge2,4,5, A.A. Postma1, A.A. Kroon5,6, J.F.A. Jansen1,2,7, and W.H. Backes1,2,5
1Department of Radiology & Nuclear Medicine, Maastricht University Medical Center, Maastricht, Netherlands, 2School for Mental Health & Neuroscience, Maastricht University, Maastricht, Netherlands, 3Department of Psychiatry & Neuropsychology, Maastricht University, Maastricht, Netherlands, 4Department of Neurology, Maastricht University Medical Center, Maastricht, Netherlands, 5School for Cardiovascular Disease, Maastricht University, Maastricht, Netherlands, 6Department of Internal Medicine, Maastricht University Medical Center, Maastricht, Netherlands, 7Department of Electrical Engineering, Eindhoven University of Technology, Maastricht, Netherlands
Intracranial vessel wall alterations may lead to an increased blood flow pulsatility and the enlargement of perivascular spaces (ePVS). To examine the relationship between these measures, this 7T MRI study applied phase contrast MRI to measure blood flow velocity in the middle cerebral artery and lenticulostriate arteries (LSAs) and obtained ePVS visual rating scores. An increased LSA pulsatility index was found to be related to a higher number of ePVS in the basal ganglia and centrum semiovale. These findings are in support of underlying alterations of the cerebral small vessel wall, which influence both the ePVS and the pulsatility.
|
||
 |
0384.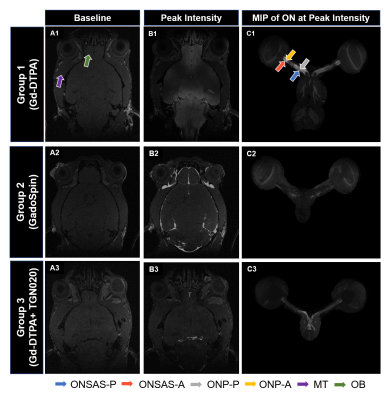 |
In vivo characterization of the optic nerve glymphatic system
Muneeb A Faiq1, Vishnu Adi1, Anoop Sainulabdeen1, Sophia Khoja1, Carlos Parra1, Giles Hamilton-Fletcher1, Choong H Lee2, Jiangyang Zhang2, Gadi Wollstein1, Joel S Schuman1, and Kevin C Chan1,2
1Department of Ophthalmology, New York University Grossman School of Medicine, New York, NY, United States, 2Department of Radiology, New York University Grossman School of Medicine, New York, NY, United States
To date, it remains unclear if a functional glymphatic system exists in the optic nerve (ON), partly because of limited in vivo methods for characterizing the cerebrospinal fluid (CSF) dynamics in the deeper brain regions. Here, we measured the spatiotemporal profiles in the ON using contrast-enhanced MRI after intrathecal gadolinium infusion, and observed indications for the existence of a molecular size-dependent and aquaporin-4 (AQP4) modulated glymphatic-like system in the ON. These findings may provide imperative insights into the waste clearance mechanisms of the visual system in health and disease.
|
|
 |
0385.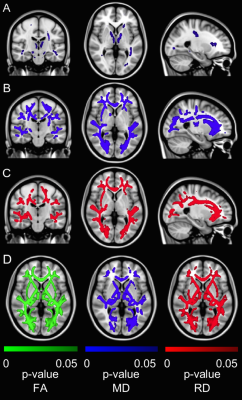 |
Cardiac disease may exacerbate age-related white matter disruptions: improvements are feasible after cardiac rehabilitation
Stefan E. Poirier1,2, Neville Suskin3, Keith S. St. Lawrence1,2, J. Kevin Shoemaker4, and Udunna C. Anazodo1,2,5,6
1Lawson Imaging, Lawson Health Research Institute, London, ON, Canada, 2Medical Biophysics, Western University, London, ON, Canada, 3Cardiology, Western University, London, ON, Canada, 4School of Kinesiology, Western University, London, ON, Canada, 5Clinical Neurological Sciences, Western University, London, ON, Canada, 6Research Centre for Studies in Aging, McGill University, Montreal, QC, Canada
White matter (WM) degeneration is associated with cognitive impairment in coronary artery disease (CAD). We used diffusion tensor imaging to assess WM integrity in brains of CAD patients before and after cardiac rehabilitation (CR) and in young and old healthy controls (HC). Widespread WM changes were observed between older and younger HC, while robust WM changes were observed in WM regions linked to cognition in CAD patients at baseline with improvements following CR. In CAD, disease manifestation and brain aging may contribute to changes in brain WM macrostructure with potential influence on cognition, and these may be quelled by CR.
|
|
 |
0386.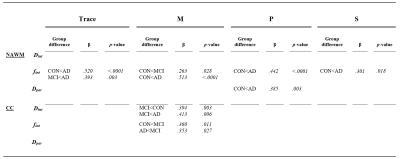 |
An interstitial fluid proxy of altered glymphatics in Alzheimer’s disease: the necessity of three-directional intravoxel incoherent motion
Merel M. van der Thiel1,2, Whitney M. Freeze2,3,4, Joost de Jong1,2, Inez H.G.B. Ramakers2,4, Walter H. Backes1,2,5, and Jacobus F.A. Jansen1,2,6
1Department of Radiology and Nuclear Medicine, Maastricht University Medical Center, Maastricht, Netherlands, 2School for Mental Health & Neuroscience, Alzheimer Center Limburg, Maastricht, Netherlands, 3Department of Radiology, Leiden University Medical Center, Leiden, Netherlands, 4Department of Psychiatry and Neuropsychology, Maastricht University, Maastricht, Netherlands, 5School for Cardiovascular Disease, Maastricht University, Maastricht, Netherlands, 6Department of Electrical Engineering, Eindhoven University of Technology, Eindhoven, Netherlands
The interstitial fluid fraction assessed with spectral analysis in intravoxel-incoherent motion MRI can be a potential, non-invasive method to identify tissue damage on a microscopic level and to investigate glymphatic alterations within different disease states. The current multi-dimensional approach has a long acquisition time, thereby lowering the feasibility of IVIM as a measurement of ISF in clinical practice. This study simultaneously investigates potential group differences in the ISF-fraction in Alzheimer’s disease, mild cognitive impairment, and controls, and explores the possibility to shorten acquisition time drastically by examining the contribution of individual primary directions.
|
The International Society for Magnetic Resonance in Medicine is accredited by the Accreditation Council for Continuing Medical Education to provide continuing medical education for physicians.