

BY MATHIEU BOUDREAU
The September 2016 Editor’s Pick is from Manuel Murbach and Niels Kuster, researchers at the Foundation for Research on Information Technologies in Society (IT’IS) in Zurich. Their paper presents a simulation-based approach to evaluate the safety of the radiofrequency field (RF) shimming in magnetic resonance imaging (MRI). Current safety standards typically call for the whole-body averaged specific absorption rate (wbSAR) – a measure of the total RF power absorbed by the human body – to be limited to 4 W/kg, and assume that the thermoregulation capacity of the scanned patient is normal. However, new generations of MRI systems support RF shimming operating modes that may induce local SAR values that might be hazardous for patients with impaired or dysfunctional thermoregulation, increasing the risk of tissue damage after long scanning sessions. Manuel and Niels’s simulation study used the Virtual Population (ViP) human models to assess different RF shimming modes in several anatomical regions, and they’ve established safety recommendations for scanning patients with impaired thermoregulation. We recently spoke with Manuel and Niels about their project.
MRMH: Please tell us about yourselves and the IT’IS Foundation.
Manuel: I did my PhD studies in MRI safety at IT’IS and ETH Zurich, and I am currently working as a project leader there.
Niels: I’m the founding director of IT’IS, which was established in 1999 with the support of the ETH Zurich. The objective was twofold: to create a flexible institute that can quickly respond to technology-related safety concerns by providing science and engineering solutions to mitigate risks, and to act as a bridge between academia, regulators, industry and the clinics. Our core competencies are electromagnetics and computational life sciences.
MRMH: Can you give us a brief overview of your paper?
Manuel: The overall goal of this paper is to assess the SAR distribution and the related thermal safety of patients who are undergoing MRI scans with simulations. One current issue is that new MRI systems have parallel RF transmit capability, which leads to much more focused RF energy absorption patterns in the body. We wanted to develop a robust simulation method to evaluate thermal safety for MRIs that use parallel transmit to shim the RF field. Our first approach in the paper was to model the local temperature increase that occurs with RF shimming.
MRMH: What do you mean by “RF shimming”?
Manuel: So, in our case, we’re shimming the B1 field, also known as the transmit RF field, which is approximately 128 MHz at 3 T. To improve image quality, many vendors implement RF shimming, which applies a different polarization configuration instead of the standard circular polarization. With RF shimming, you can increase the quality of the B1+ field inside the body, which results in better image quality. However, doing so also changes the RF absorption patterns in the body, which is what we investigate in this paper. Until now, most papers interested in RF safety only use circular polarization.
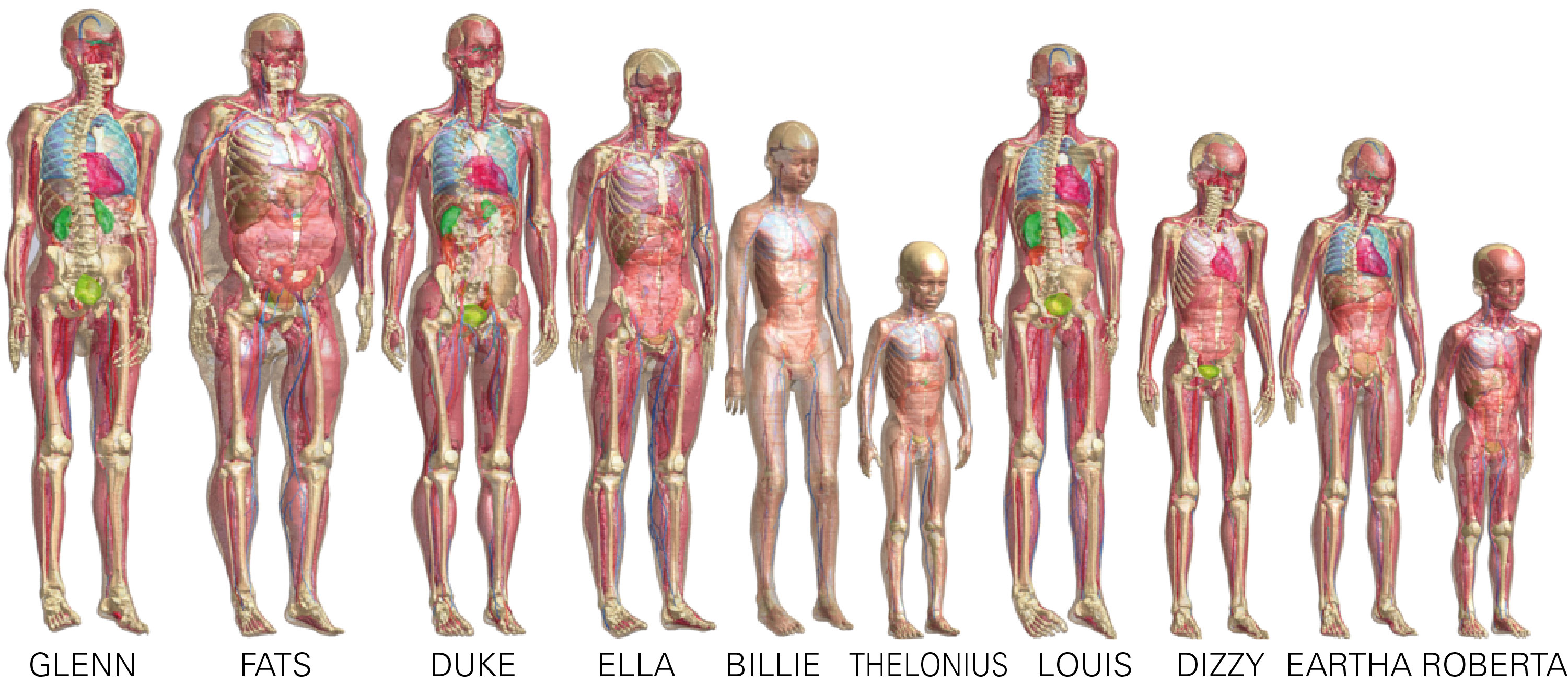
The Virtual Population (ViP) human models.
MRMH: How did you use simulations to investigate the thermal safety of RF shimming in humans?
Manuel: We used the ViP human anatomical models. The models range in size from a little girl to an obese adult, so they have quite different absorption patterns. In addition, we investigated how much RF exposure can be safely tolerated by patients with impaired thermoregulation, such as the elderly and diabetics. These patients have a limited ability to increase the local blood flow when heating occurs, so they tolerate less RF absorption safely.
MRMH: Some of our readers may not be aware of the ViP models. Could you explain what they are, and what their limitations are?
Manuel: These are highly detailed whole-body virtual human models that have been widely used for dosimetric and biomedical computer simulations. In the modeling world, most people know Duke and Ella, who are probably the two most famous models and part of the Virtual Family, but the ViP has grown since then to a broader set of models, the Virtual Population.
MRMH: And they are all named after legendary jazz artists, right?
Manuel: Yes, exactly [laughs].
Niels: We started developing the Virtual Family in 2005 for the mobile phone industry, which at the time was challenged with demonstrating that mobile phone use is safe for all users. The original Virtual Family was then expanded with the child models of the Virtual Classroom and later with obese, elderly, and paediatric models. All models are based on real MRI scans of people, have 1 millimeter slice thickness, and are segmented with semi-automated tools and functionalized with tissue models. Because of resolution limitations, the models don’t yet have complete vascular structures or sufficient detail in neural tissues, but we are in the process of adding these features. We want to push this concept into the world of virtual clinical trials.

Manuel (left) expounding on topics other than MRI safety with Niels (right) and colleague Parisa Fallahi (center) late into the night at the IT’IS Foundation 2016 annual retreat at a remote winter resort in the Swiss mountains.
Manuel: And of course in terms of MRI safety, simulations are indispensable to see what is going on inside the body – you cannot insert probes inside human volunteers.
MRMH: What did you conclude from your study?
Manuel: We concluded that if you use the RF shimming mode, it is possible to end up with a configuration that leads to very high local SAR values. If the patient has impaired thermoregulation, they may not be able to tolerate the first level operating mode due to high local temperature increases. This can be avoided by staying in the normal operating mode or in the circular polarized mode.
Niels: The study also confirms that the safety standards that are used today are insufficient and need to be revised, especially as providers are moving forward with future generations of MRI systems that have multi-port RF shimming capabilities.
MRMH: Did anything surprise you over the course of this study?
Niels: I think the biggest surprise is the discrepancy between the shortcomings of the current safety standard and the incident rate of reported hazards. Since the safety standard is practically never fully exploited with respect to maximum SAR, little happens.
Manuel: Yes, the standard would allow us to apply RF exposure of 4 W/kg constantly for an hour. This would put an extreme RF load on the patient. And although you would be allowed to do that, nobody actually does it because of safety margins and interruptions between the scans. The overall average wbSAR is maybe around 1.5 W/kg, instead of the 4 W/kg that is allowed. But, it’s kind of an unholy situation if you have a standard that allows a lot of exposure but no one uses it fully, and then they claim the standard is safe. It’s not the standard that’s safe, it’s the usage pattern that makes it safe. So we should adjust the standard.
